CDI & Clinical Documentation Software for Better Outcomes
CDI (Clinical Documentation Improvement) software is a medical software designed to improve the accuracy and efficiency of clinical documentation reporting and storage.
CDI is particularly useful medical software for emergency physicians and other healthcare professionals who need to quickly document patient information in high-pressure situations, such as bed allocations.
CDI software development is a rapidly growing field, with many clinical documentation improvement software vendors competing to create the best solutions for healthcare providers. CDI software vendors typically offer a range of features, such as automated documentation suggestions, real-time feedback on documentation quality, and tools for coding and billing optimization.
Overall, CDI software is an important tool for healthcare providers looking to improve the quality and accuracy of their clinical documentation and deliver better and faster patient care. By using these tools, healthcare organizations can improve services, reduce the risk of medical errors, and optimize revenue through more accurate coding and billing practices.
In this article, we will explore ways to improve clinical documentation, CDI for emergency departments, and EMR software integration for clinical documentation software. We’ll also discuss the unique value proposition of improving medical documentation for bed status denials with EvidenceCare’s software, AdmissionCare, for emergency physicians and hospitalists.
Medical Software for Doctors
Medical software programs provide a range of benefits for doctors and healthcare organizations. Clinical Documentation Improvement (CDI) software is designed to help doctors improve the accuracy of their medical documentation. CDI is often used in hospitals to help streamline operations so healthcare teams can easily access patient records and medical histories, as well as track patient progress and share information quickly. As a result, hospitals are able to provide better care and reduce patient wait times.
The Benefits of Digitization
Using medical software to digitize processes also enables doctors to streamline their workflows, which saves time and releases them to spend more time on patient care. This can be especially critical for emergency units, overstretched hospitals and health systems, as well as private practices.
EHR and EMR – What is the Difference?
Medical software used to document and track a patient’s medical chart(s) is usually known as an Electronic Health Record (EHR) or Electronic Medical Record (EMR). Both terms are often used interchangeably, but there are a variety of functions they provide to medical professionals.
Both allow for easier collaboration between doctors and other healthcare providers, allowing them to store patient records in one centralized location, instead of store pieces of information across fractured systems. This decreases the likelihood of patient information being lost, accidentally deleted, or incorrectly accessed by unauthorized users.
Another major benefit of medical software for doctors is the ability to improve documentation. Documentation is essential for accurate diagnoses, treatments, and medical records. With medical software, doctors can easily access patient records and medical histories, which will make it easier to provide patients with accurate and timely care.
Better Outcomes for All
Medical software providers like EvidenceCare deliver valuable tools for doctors and health systems. They help improve documentation, provide additional security to patient data, streamline workflows, and enhance the patient experience. By investing in medical software and switching to digitized processes, healthcare organizations can ensure their clinicians provide the best possible care for their patients.
Medical software has become an integral part of the delivery of quality healthcare services, and the digitization of processes has grown across the healthcare industry in recent years.
Medical software for doctors to improve documentation results in a smoother, more streamlined workflow, and improved quality of care they can provide overall. Medical software is not limited and can be used for a variety of tasks, such as digital record keeping, patient scheduling, prescription tracking, and more.
Clinical Documentation Improvement
Clinical documentation improvement is essential for accurate diagnosis, effective treatment, and optimal patient outcomes. Administrators can improve clinical documentation in hospitals in various ways, including regular training and education of physicians and staff, and following clinical documentation improvement examples. However, using CDI software adds a layer of reassurance and protection that all data is stored safely and according to regulation.
The Benefits of CDI: Why it Matters
CDI is critical for hospital administrators because it helps to ensure that accurate and complete medical records are available for billing, coding, and reimbursement purposes.
CDI also helps to support the hospital’s compliance with regulatory requirements and reporting obligations. If hospitals store data incorrectly, it can lead to a variety of issues.
Incorrect data can result in inaccurate diagnoses, incorrect treatments, and inaccurate billing. It can also lead to patient privacy and security breaches. Additionally, incorrect data can lead to difficulties with tracking patient information and medical records, making it difficult for healthcare providers to provide the best care possible.
Examples of CDI Programs and their Functions
Accurate and complete medical records help hospitals improve the quality of care they provide to patients and ensure compliance with regulatory requirements. Hospitals can improve their clinical documentation processes with technology in a variety of ways. Clinical documentation improvement examples include hospitals that can use integrated CDI software with electronic health records (EHRs) to ensure that all documentation is accurate and easily accessible, and natural language processing (NLP) to analyze the language used in clinical documentation to ensure that it is complete and accurate.
Hospitals can also use voice recognition software to convert spoken words into electronic text and ensure that all documentation is properly captured. Finally, hospitals can use data analytics to identify areas where documentation may be incomplete or inaccurate and take steps to address any issues.
CDI for Emergency Departments
The emergency department of a hospital has a unique need for clinical documentation software. For example, when admitting a patient, bed status is used to determine the level of care a patient will receive. Therefore, it is important to have accurate information to provide the best care possible.
Clinical Documentation for Inpatient and Observation
In this scenario, clinical documentation for the appropriate bed status is critical for identifying and correctly applying the correct admission criteria for inpatient or observation status.
CDI can help ensure correct admission criteria are met, and that the appropriate bed status is used for each patient, whether inpatient or observation. This helps to dramatically reduce unnecessary hospitalizations and hospital spending, while improving patient outcomes.
CDI for Better Health Outcomes
Critically, CDI can help identify opportunities for improvement in documentation and support clinicians in their efforts to achieve better outcomes.
Providing feedback to clinicians about potential gaps in the documentation and providing guidance regarding the most appropriate documentation for the circumstances leads to improvements in patient care and treatment effectiveness.
When all relevant information is captured, and the care provided is well documented, hospital administrators can allocate funding and resources more accurately so that higher-quality care is provided for all who need it. Less time and money are spent on fixing documentation issues later in the process by revenue cycle and utilization management teams.
Overall, clinical documentation software is used to ensure that all aspects of patient care are recorded in detail and to the highest standard. This includes patient history, physical exam findings, diagnosis, treatment plans, and patient outcomes. By having accurate and complete documentation, emergency departments can better assess the severity of a patient’s condition, and provide the appropriate treatment faster and more effectively.
How Can CDI Improve Inpatient Care?
CDI ensures that healthcare providers accurately capture patient encounters, diagnoses, and treatments in a timely manner. It helps reduce errors in reporting and improve patient outcomes. CDI also ensures that all relevant information is documented in the medical record.
CDI software helps reduce the time spent on documentation, and streamline the process for better efficiency. This allows doctors more time to cultivate more personalized approaches to treatment and improves the patient experience.
This is why accurate documentation is essential for high-quality patient outcomes, and CDI helps ensure that all documentation is complete and up-to-date. With CDI, emergency departments can be better equipped to make informed decisions by providing real-time data, tracking patient progress, and streamlining document submission to provide better patient outcomes.
EMR Software Integration
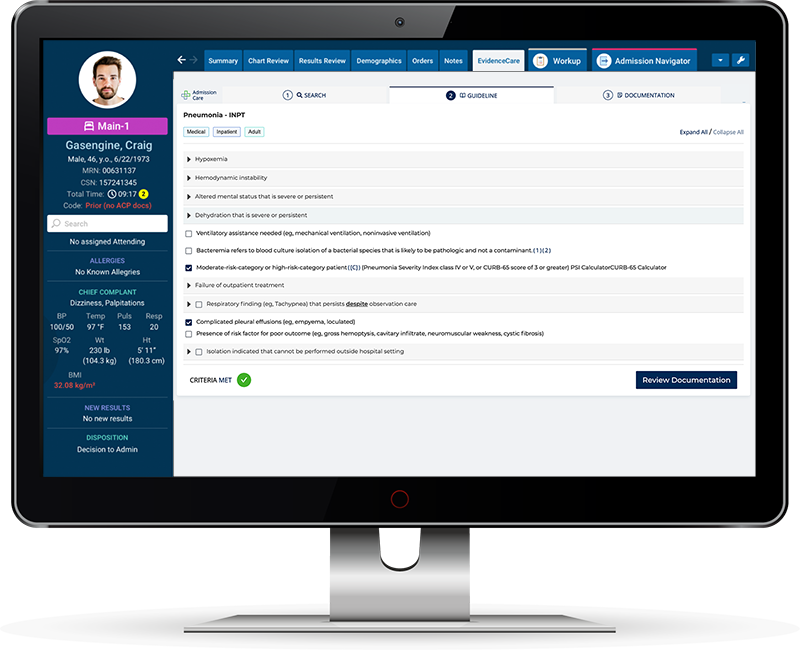
Using an EMR software integration for clinical documentation is an effective way to improve bed status decisions. AdmissionCare is a unique EMR/EHR-integrated software that helps admitting physicians and hospitalists capture accurate medical necessity documentation about bed status decisions, which is a continuous struggle for hospitals.
AdmissionCare, software for better clinical documentation of medical necessity, allows healthcare providers to document bed status criteria, automate orders into the Epic or Oracle Cerner record, and provide the information needed by Utilization Review teams. EvidenceCare’s EMR software integration for CDI improves patient outcomes, captures earned revenue, and reduces hospital costs from administrative burdens and medical necessity documentation error corrections.
Hospitals that use Admissioncare to help them manage their bed allocations consistently report:
- A reduction in medical necessity denials and documentation issues
- Faster handoffs between emergency physicians and inpatient teams
- Significant reduction in interruptions from utilization review and physician advisors
In conclusion, Clinical Documentation Software such as AdmissionCare for bed status decisions is a crucial tool for healthcare providers to manage patient information effectively. AdmissionCare not only monitors and updates criteria to stay compliant but can help providers learn that criteria over time to ensure the patient receives the best care possible.
By using Admissioncare EHR software integration for bed status criteria, doctors can greatly improve clinical documentation processes and implement CDI for emergency departments. By using integrated EMR software, healthcare providers can improve patient care, reduce errors, and optimize workflows.
Want to learn more about EvidenceCare’s clinical documentation software, AdmissionCare?
Schedule a demo today.