Reduce Variation In Healthcare
There are a few constants in the world of reducing variation in healthcare. One example is clear: “Uncontrolled variation is the enemy of quality” (Deming) and reducing less-than-ideal diagnostic and treatment methods in healthcare should be a primary goal of any health system and hospital administrator.
However, variation can be quite nuanced, and there are many types and subtypes. But what is variation in healthcare? It is helpful to ensure we agree on a definition of clinical variation before discussing it.
Clinical or care variation refers to the varying levels of care created when providers use different or non-standard methods of treatment, diagnostics, or other patient approaches compared to peers. There are key differences when it comes to reducing variation meaning. Some variations may be warranted, while others may be unwarranted.
If your goal is to reduce variation, your health system needs the right tools to understand where variation exists, what you can do to prevent it, and the difference between unwarranted and warranted.
Departures from standard medical practice will always exist, and no organization can completely eliminate them. However, you should target unwarranted variation — and subsequent differences in healthcare quality — for elimination.
Unwarranted clinical variation can be one of the biggest threats to the quality of healthcare delivery. To counter that threat, innovative health systems strive to reduce variation and improve healthcare outcomes.
There are many benefits to reducing variation in healthcare, including the following:
-
- An increase in positive patient outcomes
- A decrease in costs to your hospital
- A more predictable treatment path that allows for more targeted staff training and increased performance among clinicians
However, if you seek to be successful at reducing variability in healthcare, it’s essential to understand when it may be justified and what types of variation exist. You should also have a solid understanding of the specific causes of variation in quality, as well as what variation in medical practice and the implications for quality are.
Types of Variation in Healthcare
There are multiple types of variation in healthcare. However, the primary difference is warranted vs. unwarranted variation.
Imagine a situation in which a provider knows a patient:
-
- Responds positively or negatively to different levels of a drug
- Has a challenging lifestyle that makes one treatment method preferable
- Cannot manage a preferred treatment method
In these examples, a departure from standard care methods may be warranted.
Other times, a provider may have no valid reason for choosing an alternative option instead of standard, evidence-based treatment. In these instances, the changes can be less defensible and more problematic for the provider, patient, and health system. Unwarranted scenarios include:
-
- Outdated, over-treatment methods
- Failure to take into account patient preferences
- Inattention to new standards of care or evidence-based practices
- A lack of engagement with the patient or specific diagnostic efforts
- A preference for provider needs over those of a patient
For specific unwarranted care variation examples, consider the following clinical scenarios:
-
- Ordering a CMP (comprehensive metabolic panel) daily when there is no reason to check liver function daily and when a BMP (basic metabolic panel) would suffice. This creates increased cost to the patient.
- Ordering a BNP (b-Naturetic peptide) to determine improvement in heart failure, when a simple physical examination would give better information. This would make extra “pokes” for the patient and adds unnecessary additional cost.
- Placing patients on oxygen in the ED without a specific indication or in the Operating room (pain meds on board or patient is hyperventilating but does not “require” oxygen). This increases utilization of resources and cost of care and can also increase LOS (length of stay) if the patient is thought to have needed the oxygen, and it takes time to rule out if the patient actually has medical necessity.
- Doing routine “daily” labs, when patient is stabilized. This causes unnecessary “pokes” (patient dissatisfier) and increased cost of care.
- Duplicating studies that would provide the same information such as: Ordering carotid dopplers to evaluate plaque causing a stroke, and then ordering a CT head/neck angiogram, which is an extended study in addition to the carotids that where ordered. The alternative is to simply order the second or not do a redundant Head and Neck CT. This makes the carotid dopplers an unnecessary and redundant study.
- Getting a PET scan as an inpatient, when that information is not necessary for the diagnosis of cancer and can be done with less expense as an outpatient.
- Routine PT and OT consults on all patients because the orders are pre-checked in a providers preferential order sets. Sometimes just PT is sufficient or OT is needed for a specific condition. Also creates unnecessary consults for patients who don’t need it. This can cause discharge delays, increased cost, and overuse of resources and personnel.
There is also common cause vs special cause variation.
Common cause variation exists due to understandable or easily explained reasons, such as blood type or a patient’s fears about a specific treatment. Common cause variation in healthcare has concrete reasons and understandable explanations. You and others on your team may allow and encourage these reasons.
On the other hand, special cause variation happens randomly and for no discernable reason.
Finally, there is assignable variation in healthcare and non-assignable causes of variation. Assignable inconsistencies occur due to a specific breakdown or problem within a process. In non-assignable occurrences, these changes happen for no apparent reason.
Assignable types are always preferable to non-assignable, as you can use the right data and tools to better understand why assignable changes have occurred. However, the non-assignable type yields no additional knowledge and can be more difficult to learn from, track, and correct.
Examples of Variation in Healthcare
When considering examples of variation in healthcare, it’s important to assess the various potential causes.
There are numerous examples of random variation in healthcare. These include:
-
- Patients respond differently to identical courses of treatment due to their unique physiological makeup.
- Two doctors prescribe two different treatments to a nearly identical patient when both treatments could be equally effective or impactful.
- A doctor prefers one diagnostic method over another due to personal experiences.
There are also many unwarranted variation in healthcare examples. These unwarranted variation examples can involve the following:
At times, warranted variations in healthcare may be undertaken. These variations occur when there is a deviation from standard healthcare treatment or diagnostic methods. However, the reasons for these departures from standard practice are based on science or out of respect for patient preferences. Examples include:
-
- A doctor ignores accepted prescription guidelines because they know a patient has had adverse reactions to similar medications in the past.
- A practitioner increases or decreases the schedule of a certain therapy over a few weeks to accommodate the patient’s work schedule.
- A patient expresses a preference for a certain type of diagnostic method.
It’s essential to understand the reasoning behind alternative approaches to treatment or diagnosis. If you know the reason, you can track the source of the different approaches, determine if the changed approach was justified, and use appropriate data tools to reduce alternative approaches when appropriate.
How to Reduce Clinical Variation
Every hospital or health system should seek to reduce variation. It involves multiple steps.
First, determine what part of your healthcare team contributed to the changed approach. You can gather this information with a robust data-gathering tool that enables your hospital to ask the right questions and develop customized solutions.
Each person involved in the patient care process has a role, and your organization must ask each class of medical professionals different questions to track down potential treatment and diagnostic inconsistencies. For example, How can doctors help reduce variation? How can nurses contribute to decreasing variation in their professional practice?
Once you determine where variation occurs — and who is most likely to be responsible for the variation — you can begin to reduce unwanted clinical variation. Specific steps you can take include:
-
- Using data tools to determine which clinicians are most likely to engage in unwarranted clinical practices, then addressing those deficiencies with the individual clinicians.
- Identifying improvements you can make at the system-wide level. These improvements may include providing additional training opportunities, purchasing more up-to-date equipment, and developing a system that makes clinicians aware of their varying approaches.
- Identifying potential blocks at a system-wide level that leads providers to stray from acceptable standards of care. For example, are some treatment methods more cumbersome than others? Are there hospital conditions, equipment, or processes contributing to outdated treatment methods? Can your health system make improvements to reduce these obstacles?
- Examining specific causes or departments in which alternative approaches and treatment methods are most likely, then determining what changes you can make to improve that process.
- Evaluating socio-economic determinants of healthcare. Doing so may enable you to figure out how to ease patients’ burdens to healthcare access and identify root causes that drive varying approaches in healthcare.
There are many benefits to controlling variation in healthcare that extend well beyond positive health outcomes and reduced costs. It may even improve your hospital’s reputation and reduce legal liabilities.
Healthcare Variation Software
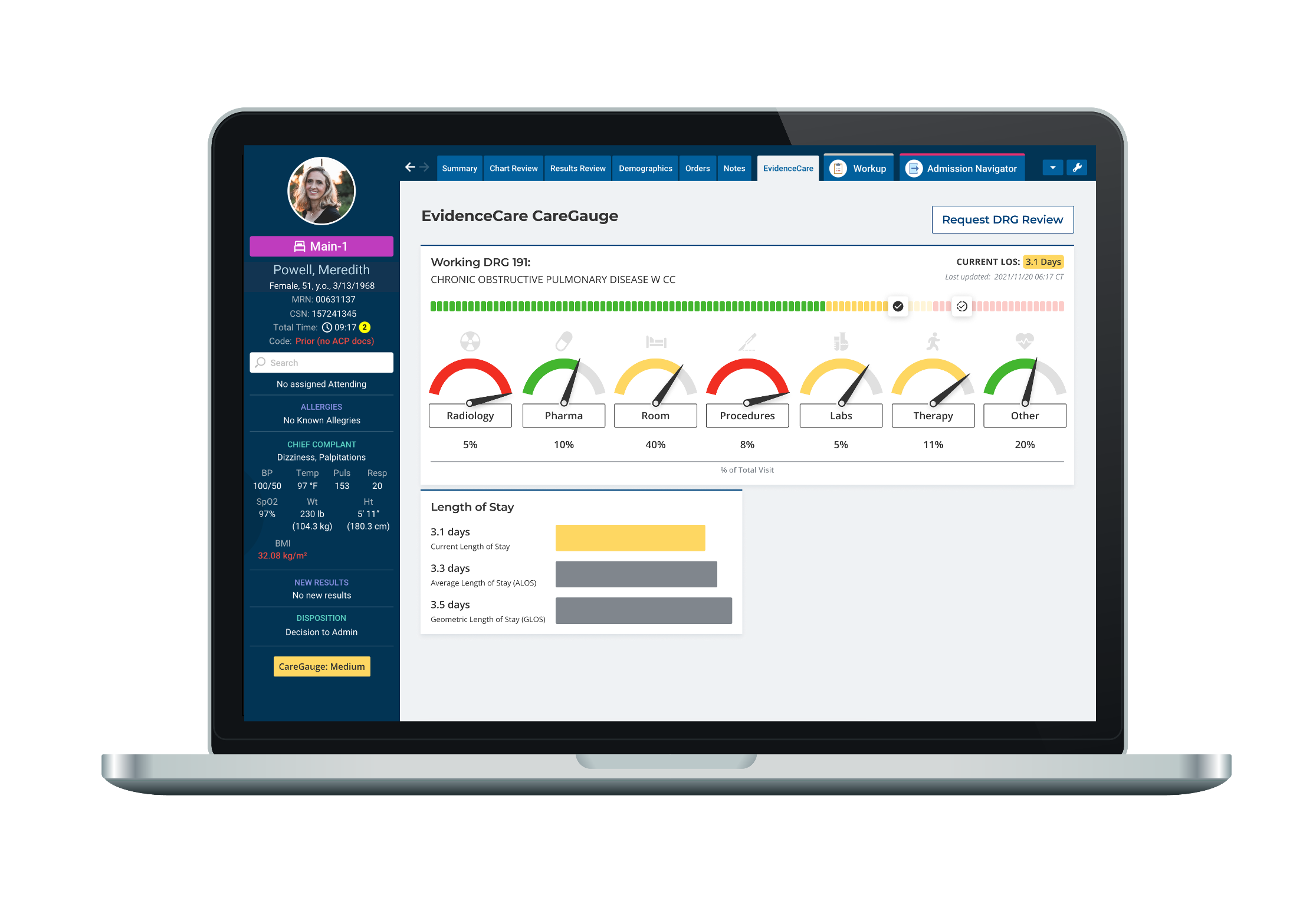
The appropriate healthcare variation software — such as CareGauge — can be critical in helping you determine the sources of these different treatment modalities and ensure you minimize differences wherever possible. However, for clinical variation software to work, it must be able to examine multiple data points, provide real-time insight, and ensure you’re using all necessary data.
Any care variation software you purchase should accomplish the following:
-
- Provide doctors a real-time view of what’s happening in their facility and generate accurate, actionable reporting to hospital administrators. This information should include critical data points on length of stay, cost of treatments and labs, and what diagnostic tests practitioners use.
- Integrate with electronic health record (EHR) systems to provide insight to doctors where they’re already making orders. The software should be as intuitive and non-invasive as possible, allowing a provider to easily observe and ignore if variation is warranted.
- Be able to track the specific costs of each patient, but also “zoom out” and obtain a system-wide perspective and comparison.
- Provide immediate feedback to the provider, enabling doctors engaged in treatment options to immediately detect unwarranted modes of treatment and adjust patient care accordingly.
Are you ready to explore the right options and purchase clinical variation software to help your hospital or health system?
At EvidenceCare, we offer software that can help you obtain broad-based and individualized causes of variation in healthcare. Our healthcare variation reduction software, CareGauge, is a major asset to hospitals by helping them find the causes of healthcare variation and identify specific reduction methods.
Contact us today to schedule a demo.