Clinical Variation
Every healthcare system will have some sort of variation. Examples of variation in healthcare are wide-ranging and can include an array of different treatment options, diagnostic procedures, and medication dosages.
There are always reasons for warranted variation. Warranted clinical variation is essentially unavoidable, as all doctors, nurses, and other practitioners have a different understanding or insight into a particular problem in a patient’s diagnosis.
This type of variation in health care isn’t a bad thing. Indeed, as long as the variation occurs within certain parameters, it can actually be a good thing. Variation allows practitioners to use their expertise to understand what works and what doesn’t for specific patients.
However, broad ranges of clinical variation can be more problematic. Most define clinical variation as the overuse or underuse of certain therapies, treatments, or diagnosis materials in a way that potentially hurts patient outcomes or the sustainability of the health system. Unlike warranted variation, unwarranted variation in healthcare is much more problematic.
As such, when considering what clinical variation is in healthcare, one must consider broader impacts. Yes, medicine isn’t exact, but medicine does operate within accepted and tested parameters. Failing to operate a practice within those parameters can be hugely problematic for patients and a health system.
Managing clinical variation is an expensive and complicated concern for hospital administrators and practitioners. You must strike a balance between trusting your doctors to act in the best interests of a patient and overusing resources in the health system.
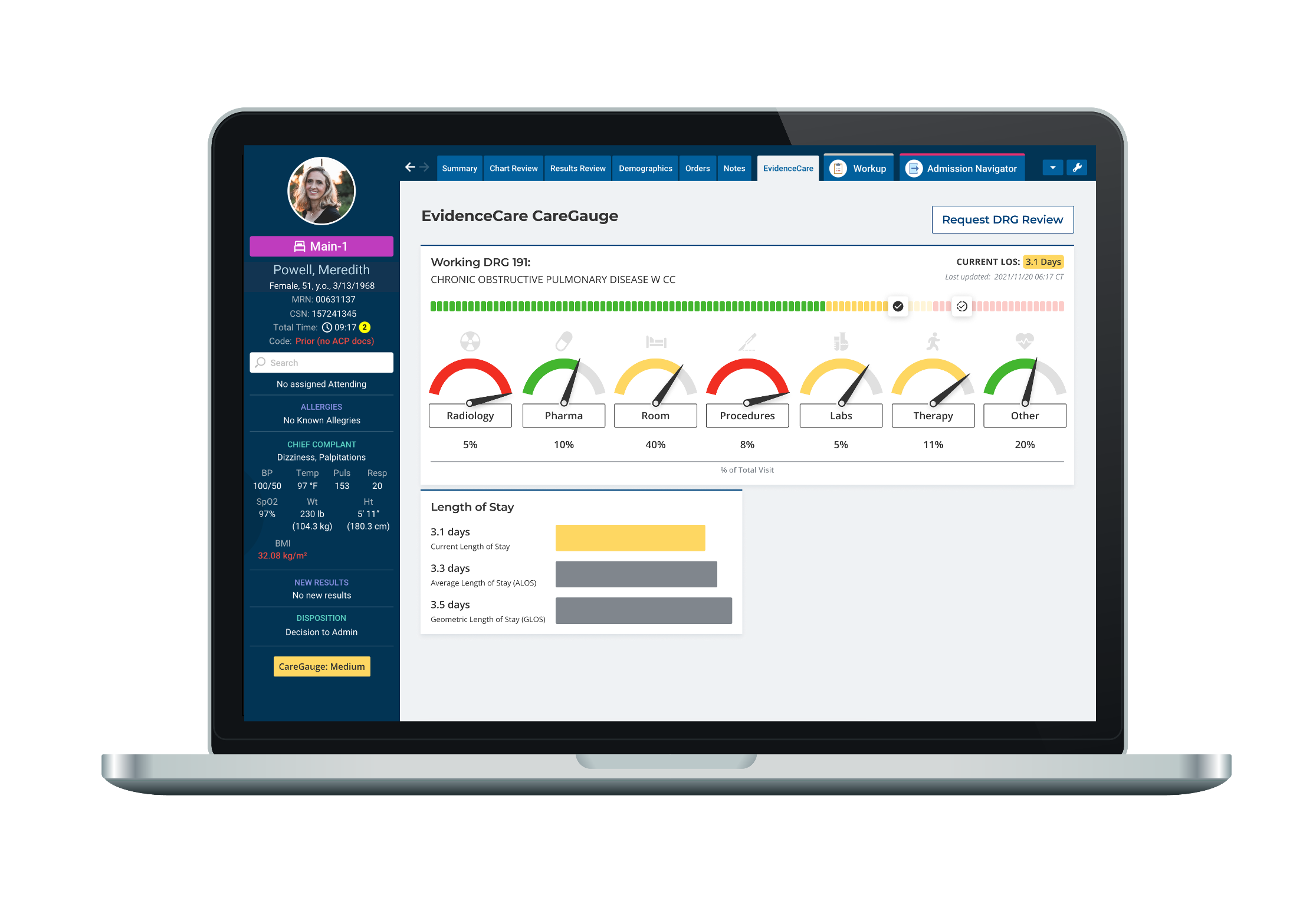
Thankfully, various tools can help individuals in charge of hospitals and health systems ensure their staff is operating within expected guidelines in terms of clinical variation. One such example is CareGauge, an EHR-integrated software provided by EvidenceCare.
When used properly, CareGauge can provide real-time data to doctors about care utilization, costs, and the effectiveness of certain treatments at the point-of-care.
Unwarranted Variation In Healthcare
As discussed, warranted variation in healthcare is good, necessary, and can improve patient outcomes. After all, the last thing any hospital administrator ever wants to do is handcuff a doctor’s intuition and knowledge to the point that they are terrified to operate outside of prescribed norms, even if such a treatment may be necessary.
Why might a doctor need to consider variations in medical practice and the relevant implications for quality? There are many examples, including:
- Consideration for the patient’s medical acuity and past history
- Fears that a patient may not be competent enough to describe their symptoms, leading to a need to obtain additional diagnostic measures that can potentially capture more information than the patient is relaying
- Concerns over the potential financial impact that a treatment or diagnostic method may have on a patient lead to a need to embrace alternative approaches
- External factors in the hospital, such as a drug shortage or an ongoing pandemic
In these instances, variation may be perfectly reasonable and warranted, and it is important to consider these factors — and more — when determining clinical variation. As such, the greater challenge is eliminating not warranted variation but unwarranted variation in healthcare. In these instances, you’re not just dealing with slight changes to accepted modalities but large outliers that lead to different outcomes and treatment methods.
Unwarranted variation in healthcare takes many forms, but at its core, it means deviation from accepted norms in such a way that will either endanger patient health or lead to major financial expense for the healthcare system. It is not enough to avoid these challenges: A hospital or health care system must actively protect their margins and reduce this type of variation.
Clinical Variation Examples
Physicians reading this could probably come up with a slew of clinical variation examples, but here are a few that may help distinguish between warranted and unwarranted variation:
- Imagine a scenario in which a patient needs physical therapy, and the normal course of treatment involves one session a week for ten months. Let’s say the hypothetical patient could not meet their obligations due to an upcoming move across the country. In that case, it may make more sense to double the weekly sessions and complete the treatment in half the time.
- Two patients may have major hip problems that require treatment. In one case, a doctor may prescribe a total hip replacement. In another, a doctor may prescribe lifestyle changes, supervised exercise, or physical therapy.
- A doctor may alter the dosage of a certain pain relief drug given to a patient, depending on their reaction to that drug. One doctor may elect to give the patient a higher dose, while another may prefer a lower one, with a gradual increase, depending on the patient’s tolerance of the drug.
At the same time, plenty of unwarranted variation examples can demonstrate the harm it can cause in health care. Consider the following:
- If a doctor prescribes five times the recommended drug amount to a patient, despite the lack of evidence for the clinical effectiveness of the increased dosage.
- A doctor fails to prescribe physical therapy to a patient after major surgery, despite all indications being that the patient will benefit from such therapy and that there are no financial or socio-economic constraints on the patient.
- In some cases — such as depending on the location of the hospital — patients may be more likely to receive certain treatments, despite the total lack of any evidence that the treatment is more or less effective.
Reducing Clinical Variation
Reducing clinical variation is critically important to doctors, patients, and healthcare systems in general. Clinical variation reduction and an increased reliance on evidence-based treatments and tools results in improved patient outcomes, enhanced quality of life, and reduced hospital admissions.
Reducing variation in healthcare can have a massive impact on health systems. Clinical variation often results in unnecessarily defensive medicine. This can lead to unnecessary costs that don’t ultimately add any value to the patient’s health outcome.
There are many ways that practitioners and healthcare networks can reduce clinical variation. One such example is a clinical decision support system.
A clinical decision support system is meant to give practitioners advanced and potentially pre-programmed knowledge that can help guide care and diagnostic decisions for a patient. In their ideal form, they can help medical professionals determine the best course of care for patients.
Clinical decision support systems have many advantages, including:
- A wide range of flexibility. Hospitals and health systems can use a knowledge or non-knowledge-based clinical decision support system, depending on their needs and the resources available. This can enable a health system to better incorporate advanced clinical knowledge.
- The ability to protect patient safety. By ensuring that practitioners operate within acceptable variation limits, a CDSS can ensure that patients are being cared for in accordance with the best evidence and models possible.
- Increased efficiency. When used properly, a CDSS can operate within an EHR, ensuring that doctors can easily integrate their decision-making within systems already in use. This allows practitioners to work with maximum efficiency while also ensuring that they are making patient decisions that ensure the best clinical outcomes.
When used properly, a CDSS can standardize care and reduce unwanted clinical variation. There is emerging CDSS software specifically focused on reducing care variation.
Clinical Variation Software
In its ideal form, clinical variation software contains many benefits, including:
- Provide a top-down and individualized perspective on care utilization and how each practitioner uses care. This enables hospitals to see how patients are responding to care, as well as how practitioners prescribe it. As such, a hospital can use clinical variation technology to identify problematic behaviors and address them before they become too ingrained or cause a major health challenge to a patient.
- The opportunity to track numerous metrics, including length of stay, therapies prescribed, and diagnosis methods used to make a final diagnosis.
- Cost comparisons can determine how each doctor’s individual approaches cost the hospital, particularly when balanced against broader margin issues.
To operate in the best way possible, clinical variation reduction software must contain numerous facets, including:
- The ability to reduce variation with clinical decision support. In other words, such a program must integrate with clinical decision support software in order to provide a comprehensive perspective on clinical variation within a practice.
- Integration with an EHR system, as well as a customized ability to integrate with other HIPAA-compliant software
- Provision of real-time feedback that can immediately alert practitioners and administrators about how their variation compares to others. Real-time feedback can enable immediate changes in behavior that can better drive decision-making in the future.
- Constant updates that are evidence-based and evolve with changing technology and medical breakthroughs. A system that is out of date and not immediately updated with newly available research won’t meet the needs of modern patients, potentially endangering patient safety and exposing the healthcare network to legal liability.
As you can see, the clinical variation reduction software you get needs to meet multiple requirements for maximum efficiency. EvidenceCare’s CareGauge offers all of these benefits and more.
Are you ready to learn more about how CareGauge can reduce variation in real-time in the EHR?
Contact us today to schedule a demo.