Optimizing Patient Care: Understanding and Managing Hospital Length of Stay
Hospital length of stay is a patient’s duration from admission to discharge. Different hospital admissions exist, including emergency, holding or observation, direct, and elective admissions.
Emergency admissions bypass the usual protocols owing to the severity of the patient’s condition. It could be a life-threatening heart attack, a near-fatal car accident, gunshot wounds, or the aftermath of a natural disaster.
Holding or observation admissions are for patients that require diagnostic tests. Patients in this category may stay in the hospital for 24 to 48 hours. Conversely, direct hospitalizations occur when a doctor must admit a patient they’ve attended to before.
Elective admissions comprise a significant portion of hospitalizations. They happen when a patient requires surgery or further treatment, but the patient already knows about their health condition. Doctors reserve hospital beds for such patients on stated dates and can change the date if the situation allows it.
That’s a sneak peek and helps elaborate on the meaning of length of stay. By monitoring how many days a patient spends in the hospital, administrators can gauge the efficiency of healthcare services. Hospitals strive to offer quality care while minimizing the length of stay.
Why is the length of stay important? Prolonged stays are expensive for the patient, hospital, and insurance providers. In addition, it impacts hospital readmission rates, i.e., the frequency at which a hospital readmits patients after their initial discharge.
Extended stays disrupt a patient’s ability to transition from hospital to home care. Moreover, chances are high that patients will suffer from hospital-acquired conditions (HACs). These are complications like pressure ulcers and infections.
So, focusing on length of stay reduction ensures hospitals remain efficient and can also improve outcomes. Hospital readmission penalties adversely impact revenue, and their avoidance is crucial. It is, therefore, important that hospital leadership monitors these numbers.
Average Length of Stay
Average length of stay (ALOS) calculations help assess patient flow and resource allocation. The outcome of these calculations is a key performance indicator (KPI) for the patient management team. Through hospital ALOS, the team can keep tabs on durations. Any outliers are quickly addressed, and the best decisions are made.
How do you calculate ALOS? The average length of stay formula comprises two parameters, i.e., patient days and patient numbers. Take the total length of stay divided by the patient numbers in the period under consideration. Here is a better expression of the formula:
The average length of stay = Total length of stay / Number of patients
To illustrate, let’s assume Hospital A registered patient stays of 3,000 days in January. Also, in the same month, the facility treated 500 patients. The average length of stay would be:
3,000 / 500 = 6 days
Hospitals can use the CMS length of stay benchmarks to gauge their achievement or improvement on the days.
Eurostat’s length of stay statistics indicate men have more prolonged hospitalizations than women. Children aged 1-9 also have the shortest inpatient stays compared to adults above 85.
Overall, surgical and critical care patients benefit the most from the impact of services rendered by reducing ALOS. Furthermore, hospitals with minimal ALOS have fewer post-operative complications than those with high turnaround numbers.
The average length of stay in hospital calculation also helps in pediatric care. Hospitals that keep their ALOS short create child-friendly environments while the parents express satisfaction. Moreover, the clinical team has fewer medication errors.
Hospital length of stay benchmarks are useful to address delays in hospital discharges. The delay typically results from poor discharge planning, delayed decisions, poor care management, and long waiting times.
Factors Affecting Length of Stay in Hospital
Healthcare is costly, and hospitals should avoid unnecessary admissions and reduce extended length of stay in the hospital.
Among the factors affecting the length of stay in the hospital are the following:
The Severity of Illness
Most conditions, including surgery, require diagnostic tests that may take extra time. Maternity stays are typically 1-4 days with no complications. Patients with severe injuries vary and require more time. Heart attacks and burns have varying treatment needs depending on severity and may prolong a patient’s stay.
Pre-Existing Conditions
Pre-existing conditions, also called comorbidities, require management along with the primary reason for hospitalization. There are medication regimens, treatment plans, and monitoring for possible complications, which a hospital length of stay analysis helps track.
Post-Operative Care
Surgical procedures have defined recovery periods that influence how long a patient stays in the hospital. Complex surgeries, pain management, and post-operative monitoring all extend hospital stays.
Acute Care Accessibility
Rehabilitation centers and skilled nursing facilities for patients needing ongoing care may have tight bookings. The process of securing one can be challenging and may mean patients remain in the hospital longer than necessary.
Social Factors
Patients need a restful environment back home where they can heal and stabilize. However, not all patients have such support systems, and planning can cause delays when scheduling discharges. These often fall under the category of social determinants of health that many hospitals are trying to address to achieve health equity.
Insurance Coverage
Insurance policies can impact hospital stays. Usually, medical insurance providers impose restrictions on specific treatments and procedures, and processing authorizations takes time. Collectively, policy hiccups affect medical decisions, and this trickles down to an extended length of stay in the hospital.
Other factors that can affect hospital stays include:
-
- Patient’s age
- Gender
- Marital status
- Employment
- Disease type
- Previous admission history
- A patient’s condition at the time of discharge
- Mode of paying hospital bills
- Nature of the treatment provided
Addressing these variables empowers healthcare providers to optimize patient care, improve efficiency, and process timely discharges. As mentioned earlier, the consequences of increased length of hospital stay only increase healthcare costs.
Reducing Length of Stay in Hospitals
Despite the lack of a clear-cut figure, 24 to 72 hours is the ideal duration for short stays in the hospital. But it is the extended stays that are a cause for concern. Here are some strategies for reducing the length of stay in hospitals.
Discharge Planning
Hospital teams should anticipate possible discharge dates at admission. Is it achievable? Through the involvement of nurses, physicians, and care managers, it is possible to predict when a discharge will likely take place. Length of stay software can also help predict a patient stay based on their diagnosis.
Harnessing Multidisciplinary Care
Multidisciplinary care involves tapping into every hospital resource, including specialists and finance teams. It ensures quick decisions, efficient diagnosis, implementation of treatment plans, and prompt billing. Collectively, these measures help reduce the length of stay.
Remote Monitoring
Continued medical technological innovation allows remote monitoring of patients. Physicians need not appear in person. They can conduct virtual consultations and guide nurses on the best treatment plans. In the end, patient deterioration is detected early.
Family Awareness
Families with patients in the hospital have the right to information on the treatment progress. Healthcare professionals should appraise family members on the condition of their patients. There is a need to disclose post-discharge care and ongoing treatment.
Inpatient care consumes about 30% of total healthcare costs in Europe and the U.S. On average, the length of stay is 4.5–5 days.
Patients and their families can enjoy the financial savings of reducing the length of stay in hospitals. Hospitals have their share, too, as they commit less supply, staffing, and facility costs.
When hospital authorities focus on reducing the length of stay in hospitals, they can register positive growth in the same areas. The clinical impact is the most significant. Consider when a person is admitted to a facility. The longer they stay, the longer they require clinical attention.
Length of Stay Software
Hospital length of stay software has helped revolutionize operations and patient care. Length of stay prediction software offers real-time data analytics. Physicians have access to performance indicators such as patient flow, readmission rates, and length of stay.
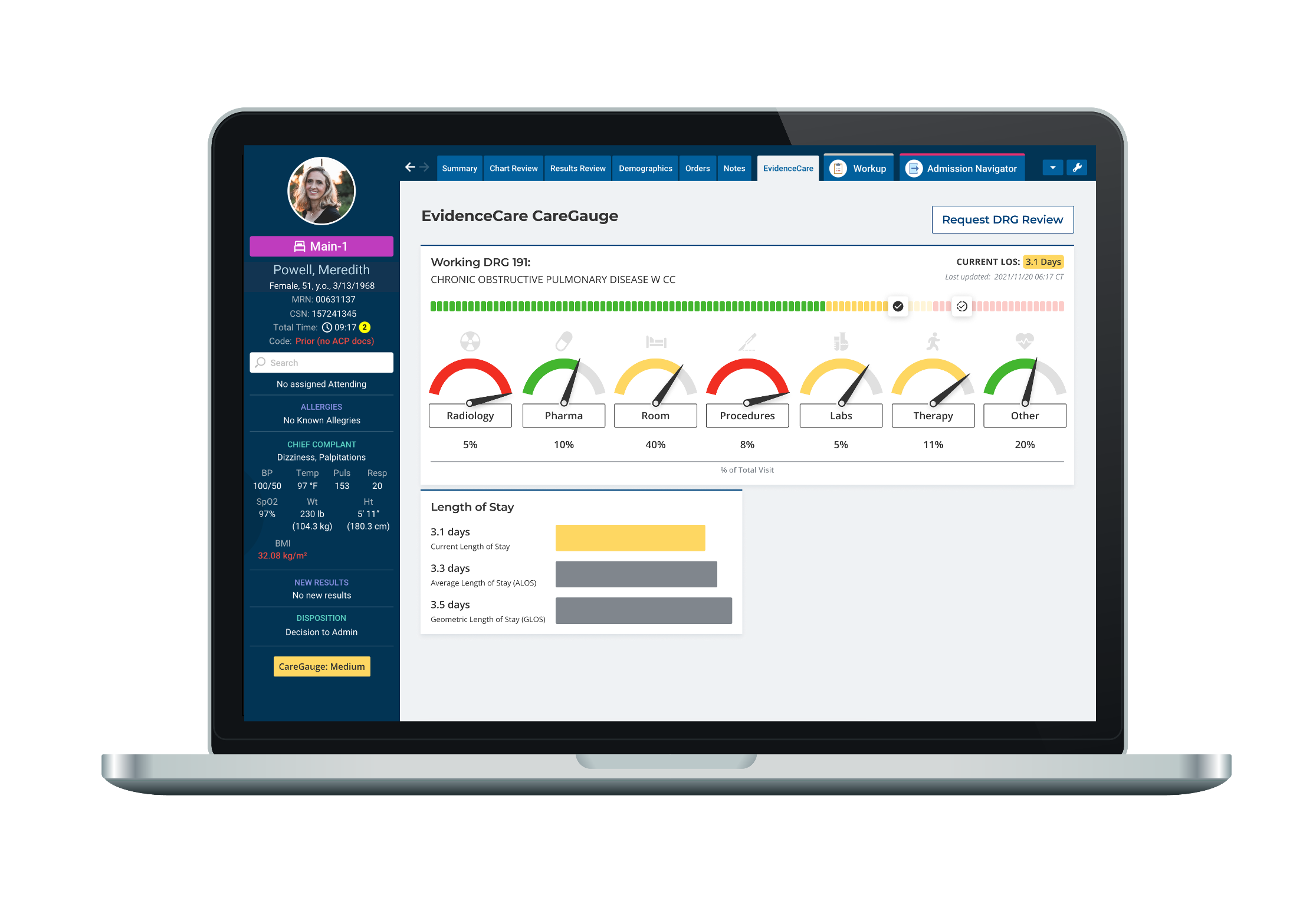
In addition, EvidenceCare’s length of stay software, CareGauge, integrates with electronic health record (EHR) systems resulting in a seamless operation. With such integration, care teams can access accurate patient data, improving care coordination and decision-making.
Discharge planning is another benefit hospitals can derive from length of stay optimization software. With this resource, care teams can quickly identify post-care options that a patient needs. Plus, the team coordinates service delivery from different sections.
Length of stay management software gives care teams a central platform to document their plans. They can share patient information and update care plans in real time. Ultimately all team members are in sync, translating to efficient service delivery.
Patients’ bed status and admission documentation is another feature clinical decision support systems like EvidenceCare address. It gives hospital admission teams the appropriate bed status and documentation at the point of admission. As a result, patient transfers take place smoothly, and there are no admission delays or reimbursement issues for hospitals.
CareGauge length of stay software helps streamline clinical workflow. The patented care variation reduction software integrates into a physician’s workflow, improving the issue of unwarranted clinical variation and high length of stay.
CareGauge shows physicians how their decisions on patient care compare to other patients with a similar condition. The software leverages historical data of patients admitted and discharged at a facility. This information serves as a benchmark for current treatment decisions.
By interacting with the length of stay reporting software, physicians obtain real-time data on medical procedures, medication, lab tests, and imaging, impacting a patient’s length of stay.
The impact of hospital length of stay on costs translates to $325 average savings per discharge. At the same time, CareGauge has the potential to reduce the length of stay by over four hours per discharge.
Schedule a demo of CareGauge today!