How to Improve Value-Based Care in Hospitals
Michael Porter and Elizabeth Olmstead Teisberg introduced the value-based care model in 2006. Since then, the model has gained traction across different healthcare systems worldwide.
Value-based care in hospitals incentivizes the quality of care providers offer their patients with improved outcomes and reduced costs. There have been ongoing discussions and legislation from CMS pushing for the focus to improve value-based care for many years.
Everyone wins when the providers aim to offer full-person and full-value health care. One of the significant benefits of value-based health care is ensuring that the patient receives good health attention at low costs, leading to effective treatment plans and positive health results.
When the focus is on the patient rather than monetary gains, value based-healthcare offers patient satisfaction. Patient satisfaction is often an essential factor to consider when measuring the quality of healthcare services. Patient satisfaction can affect clinical outcomes and patient retention.
The emphasis on quality instead of quantity enables healthcare providers to handle only small patient loads reducing their administrative burden. Also, it helps physicians to focus better on their area of expertise and offer more meaningful patient interactions.
Finally, a healthy society is a goal for value-based healthcare eliminating possible barriers to holistic care and fueling patients to have healthier longer lives.
The COVID-19 pandemic struck almost every part of the healthcare system and caused disruptions that led to an accelerated focus on costs and equity of access to healthcare.
The pandemic allowed healthcare leaders and policymakers to step back and restrategize on offering proper healthcare and cost-effectively improving patient outcomes. Let’s delve deeper and discuss more strategies to enhance value-based care in hospitals.
Value-Based Care Metrics
How does value-based care work, and how do you measure its success in healthcare? The traditional fee-for-service model focuses on volume. Value-based care metrics are a better way to measure success and focus on quality outcomes over quantity.
Measuring quality in any business is an uphill task, but using value-based care CMS regulations as a guide can increase effectiveness with more focus on patient outcomes.
The following are examples of value-based care metrics that can improve the delivery of quality care tied to the value-based care model.
Efficiency and Effectiveness
The value-based care model ensures patients receive proper care at the right time. The healthcare providers also provide this care following the correct steps.
The metrics also prevent patient readmission after treatment. It is through delivering a high level of care to ensure the physician’s assessment is accurate both short- and long-term
Timeliness and Ease of Access
Providing prompt treatment reduces barriers and improves the quality of treatment given to patients. It also increases patient satisfaction. Value-based care metrics make it easier for patients to get doctor appointments. It reduces the waiting time and gives the patient and positive effect.
Patient Focus
Patients should feel their doctors respect and are attentive to their concerns. Value-based care guidelines allow physicians to spend time with patients and answer their questions. As a result, it promotes better communication and a more fulfilling experience.
Value-Based Healthcare Examples
Payers and federal regulators can use different healthcare reimbursement models to ensure hospitals and providers stay motivated toward value-based care.
Organizations can also promote value-based reimbursement models in healthcare for higher-quality and cost-effective patient care. Here are some value-based healthcare examples to help promote quality care for all patients.
Financial Incentives
Value-based care payment models and incentives are vital components of value-based care. The payments involved here link the healthcare provider, hospital, or health system compensation on specific costs, quality, and equity in performance.
Some factors motivating the healthcare providers on the structure of these payments include;
-
-
- Upside and downside risk: Retrospective payments have an upward risk of ensuring healthcare providers are reimbursed for services already rendered. On the other hand, healthcare providers give prospective payments upfront, which is a downward risk. However, these prospective payments are value-based reimbursement for healthcare providers as they offer a more significant financial incentive.
- Timing, size, and delivery of incentives: Providers can be motivated by value-based payment model examples like financial incentives. These are given directly to them and are not delayed. The incentives here are linked to how the providers perform.
- Percentage of providers’ revenue tied to value-based payments: Available evidence shows that providers are more motivated to deliver when the value-based care payment models are connected to value-based payments.
Non-Financial Incentives
These healthcare reimbursement models encourage healthcare providers to improve the quality of their service to patients. A healthcare provider is noted as high-quality and affordable when there is good performance in value-based care.
Measurement
Reimbursement to health and hospital systems and individual clinicians depends on their performance on quality and safety. These may include death rates and timeliness in patient care.
Clinicians should ensure to offer the best possible care to patients in need and desire healing, which ignites the patients’ hope.
Value-Based Healthcare Framework
Value-based healthcare is an ongoing topic and is important enough to transform healthcare today. The healthcare value-based healthcare framework is meant to bring improvement in the health outcomes of patients all over the world.
It is a value-based healthcare model that defines the outcomes that matter to patients and the costs needed to achieve these outcomes.
Below are the elements of a value-based healthcare framework. They are the six recommended action items that must be completed prior to implementing VBC.
1. Organize Care Around Medical Conditions
Care delivery is a value-based care model organized around the patient’s medical conditions.
2. Measure Outcomes and Costs for Every Patient
After healthcare analyzes the patient, the next element involves sharing the outcomes and the costs measured for every patient’s condition.
3. Aligning Reimbursement with Value
Some reimbursement models reward healthcare providers and individual clinicians for quality outcomes and efficiency in patient care, including bundled payments.
4. Systems Integration
When defining and implementing value-based health care: a strategic framework includes the regional delivery of patient care. The provider, patient treatment, and setting should match accurately.
5. Geography of Care
These are types of value-based care models and elements that recognize complex patients and offer them excellent care.
6. Information Technology
The right information technology system is made available for identifying and supporting the significant elements of the value-based care agenda.
Value-Based Care Strategies For Hospitals
Value-based care is a provider payment that recognizes and rewards high-quality healthcare and not just the quantity of service rendered.
The goal is to improve patient lives while also managing and reducing the cost of care. Below are strategies to implement value-based healthcare. They also highlight the benefits of value-based care for patients and populations.
Identify Patients With The Highest Risk
Ensure that your healthcare facility has an EMR and integrated CDS that can identify the gaps in the care of patients. A CDS system is helpful as it transforms collected data into actionable insights. This system can identify patients and populations with high risk.
Address Patients Who Need Care
After identifying high-risk patients, addressing those who need care is one of the value-based care strategies where you can help patients who need care. Set appointments with them via phone calls, messages, and emails.
Encourage Wellness Visits
Suppose your hospital can use and assign mid-level providers to perform annual wellness visits on your patients, especially those in value-based care services. The visits can include diabetic screenings and other health assessments to help identify risk factors.
Be Open-Minded to Succeed at Value-Based Care
Value-based care strategies for hospitals include having a team focused on quality data who comes to work with your team and create a plan that addresses ways to close present gaps. It is one way for hospitals to succeed at value-based care.
Keep Open Communication with Provider Relation Reps
Hospitals should know that payers are looking into their value-based care incentive targets. Ensure that there’s an ongoing good relationship with your provider/payer representatives so that you’re always aware of what quality measures are used to score you.
Value-Based Care Software
So how does value-based care work in action? Value-based care helps payers and providers gain insights to achieve shared and set objectives.
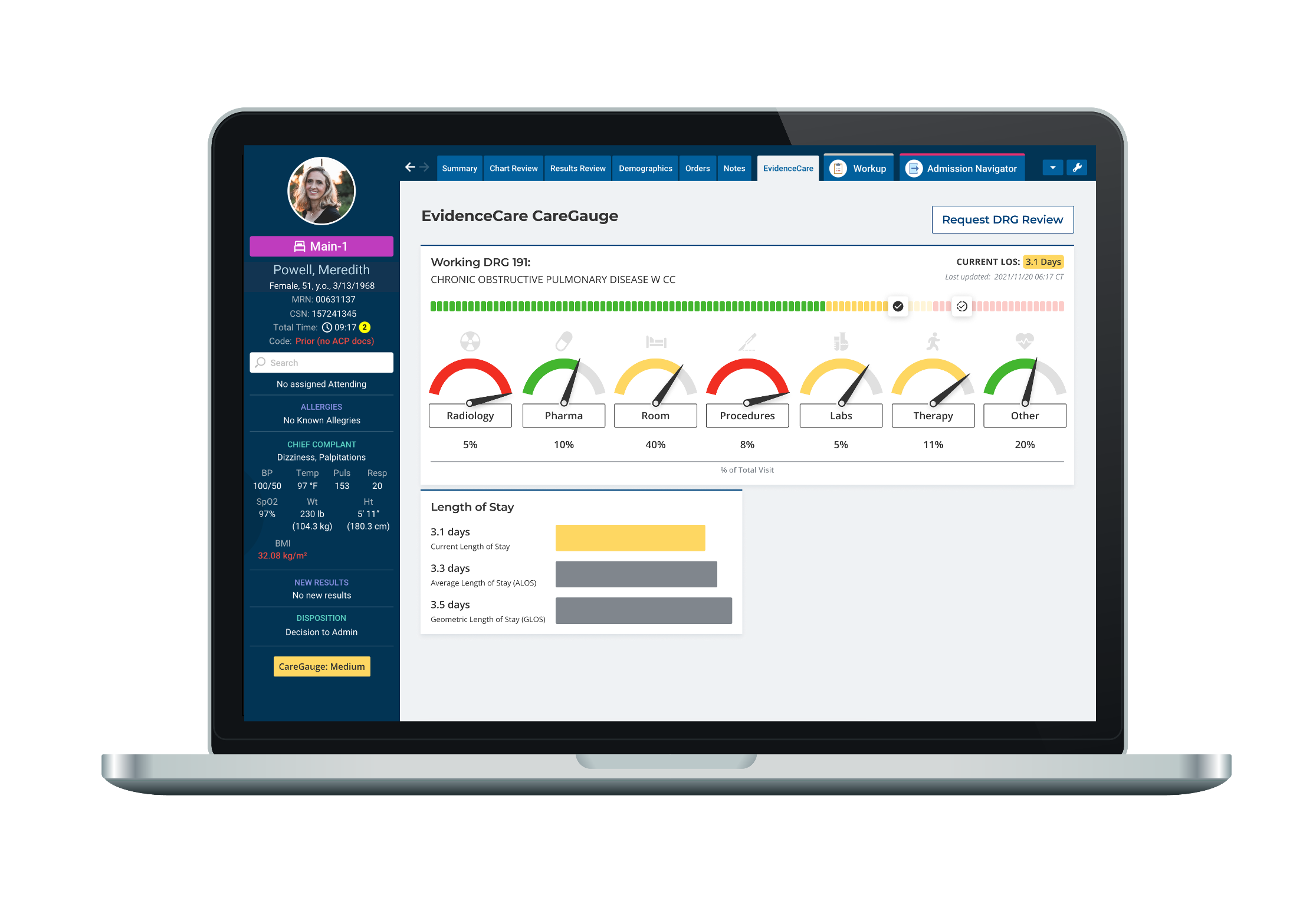
Value-based care software – like CareGauge – promotes outstanding care quality, better patient care, and cost-effectiveness. Here are more benefits of using this type of clinical decision support software.
Access Actionable Insights
The value-based care software helps you make informed management decisions without missing essential data points. These are available at the hospital, provider, and patient levels.
Achieve Transparency and Alignment
Physicians enjoy cost transparency and more visibility in their selected treatment plans. On the other hand, hospital leadership can use quality improvement software to gain insights that elevate physician practice to eliminate unwarranted clinical variation. The software promotes strategies that focus on achieving value-based care goals.
Reduce Administrative Burdens
The value-based software reduces the length of stay for patients because of the instant projections shown to providers in the EHR, and the group reports are easy and quick to build. The data visibility is immediate; you only need to upload the cost data during implementation.
Enhance Provider Engagement
Provider engagement with patients is one of the examples of value-based care.
CareGauge helps reduce clinical variation, which helps them meet the set metrics. It keeps them engaged and helps them better understand how their decisions impact value-based care outcomes.
Conclusion
When hospitals embrace value-based care, they take patient outcomes further than the hospital walls and improve the overall health of a patient. It is also a strategic move to quality healthcare while reducing costs and improving their margins.
Value-based care means keeping the patient first, prioritizing their approaches, listening to them, leveraging value-based care software, and desiring continuous improvement.
Seizing this opportunity for value-based care in hospitals will improve how providers deliver care to patients by ensuring they receive the best possible treatment during all their visits.
It also means recognizing clinicians’ and hospitals’ exemplary performance in quality care and compassion. The key is to desire better quality by remaining relentless and committing ourselves to delivering value-based care in all our hospitals. It will foster hope and healing for all patients desiring the care they need.
Contact us today to schedule a customized demo of CareGauge.