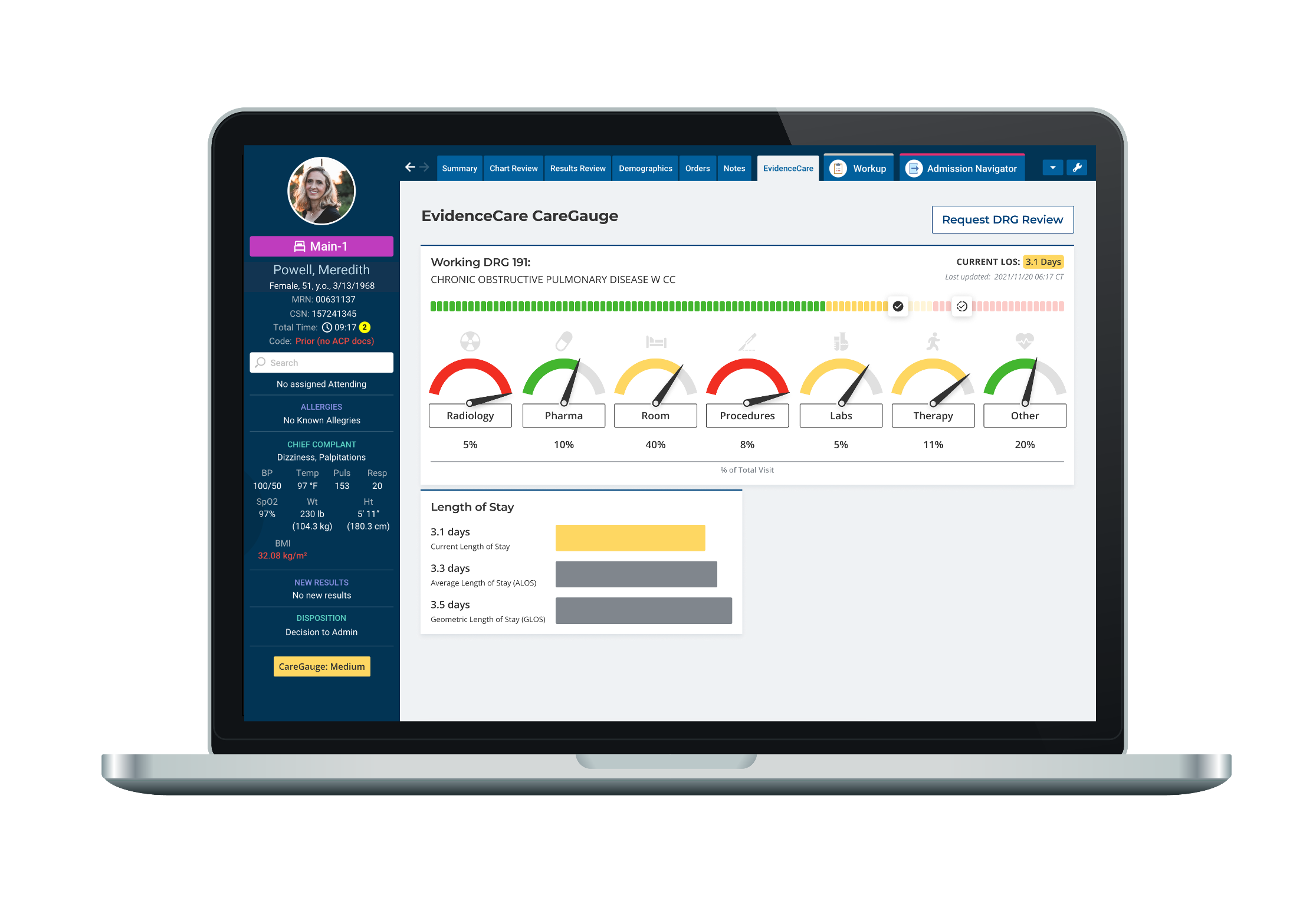
Value-Based Care LOS
Value-Based Care (VBC) is a hot topic in healthcare today, and with good reason. Let’s start with an important question:
What is Value-Based Care? Value-Based Care is a specific incentive-based model in which organizations—like hospitals—are compensated based on a patient reaching specific metrics. This practice flips a traditional payment model on its head–instead of paying hospitals for services rendered, hospitals are paid for outcomes.
Value-Based Care is often deeply intertwined with Length of Stay (LOS). Length of stay specifically refers to how long a patient stays in the hospital. It goes without saying that patients should be discharged whenever doing so can be done safely. The Value-Based Health Care Model often incentivizes healthcare networks to discharge patients at the fastest possible speed—provided discharge can be done safely and with the understanding that hospitals will be financially penalized if there are readmissions.
In this sense, Value-Based Care and LOS are deeply integrated. Safely reducing the average length of stay will often result in improved payments to hospitals.
Other critical elements of Value-Based Care include the following:
Value-Based Care in healthcare differentiates from other healthcare models because of what it tracks. In many healthcare and consumer models, payments are issued based on services provided. This can, however, result in defensive medicine and unnecessary testing in healthcare. Inappropriate financial incentives can increase healthcare costs, driving up insurance costs and ultimately resulting in additional costs to consumers.
As such, Value-Based Care incentivizes the appropriate use of healthcare services to improve outcomes. The Value-Based Care model has become widely adopted because of its ability to improve care without increasing costs.
Benefits of Value-Based Care
When used properly, Value-Based Care strategies for hospitals can significantly improve patient outcomes while also decreasing costs. In an era where everyone recognizes healthcare costs to be far too high, using Value-Based Care in hospitals has become widely accepted as a tool that can properly control rapidly increasing healthcare costs.
There are many examples of Value-Based Care that hospitals have used. These include:
-
- Bundling Medicare payments; something that’s accomplished via robust data collection
- Working with an integrated medical team that has complete access to all necessary medical records
- Standardizing medical record systems to ensure that all members of a doctor’s team have access to test results, eliminating the need for duplicate tests
These Value-Based Care solutions may seem widely disparate, but they have many elements in common: They harness data to make appropriate medical decisions about a patient’s ongoing healthcare.
Many of these solutions and strategies can be deployed by hospitals. This is particularly the case when it comes to enhancing access to medical records. An entire medical facility can standardize access to a patient’s medical care by ensuring that all staff can have the same access.
The tangible benefits of Value-Based Care cannot be underestimated. Value-Based Care can achieve better healthcare outcomes for patients at a reduced cost. They tend to focus more on the provision of preventative care, as well as focusing on non-healthcare-based solutions around social determinants of health, like transportation barriers, that promote overall health equity. In this regard, “softer” healthcare items can be extremely valuable for handling real patient health needs.
However, the intangible benefits of Valued-Based Care are often under-discussed. Value-Based Care can improve outcomes and reduce the length of stay in hospitals. Implementing this model allows healthcare teams to achieve the best of both worlds. Patients can get better healthcare but be discharged faster.
VBC Best Practices
While value-based health care has become popular of late, value-based care models are often implemented without thought to true best practices. As a result, it is vital that hospitals not only implement VBC best practices but also fully understand how to improve value-based care in hospitals.
The most important best practice needed to implement Value-Based Care is electronic health records. Robust data collection—and easy access to the data collected—is critical, as it will allow medical team members to know what tests a patient has undergone and what the test results were. This information can better inform future healthcare decisions.
This data collection is necessary to understand how payments can be bundled, a commonality when it comes to Value-Based Care. After all, you cannot bundle payments if you don’t know what tests have been completed and which are still remaining.
Improving Value-Based Care approaches requires the appropriate implementation of Electronic Health Records and integration with software like clinical decision support (CDS) tools. This plan requires the use of an experienced vendor and team who:
-
- Has ample experience in the area of EHRs and VBC
- Can implement a CDS software that follows the 5 rights of CDS and is integrated with a patient’s EHR
- Can provide trend and broader data information that shows how a hospital performs regarding individual patient metrics and clinician metrics
Using best practices—and the experience of other hospitals—can be critical in informing your VBC execution.
Average Length of Stay in Hospital
Most VBC models seek to reduce the average length of stay in a hospital, as doing so can result in major cost savings and is often regarded by payers as a key metric when it comes to making payments. The exact average length of stay in hospital formula sometimes varies, but the length of stay calculation is usually some variation on the following:
-
- Amount of time that the patient spends in the hospital
- How quickly they are discharged
- Whether or not the patient is readmitted as a result of future complications
Some hospitals also adjust their formula for Case Mix Index using DRG data. The length of stay formula is intertwined with length of stay cost savings. Safely reducing the length of stay will result in cost savings to payers and additional payments to hospitals.
These payments are usually reduced if there are future complications that may have been addressed by keeping the patient in the hospital longer. As such, hospitals are not incentivized to discharge a patient earlier than medically necessary.
However, length of stay and quality of care are related as well. It would, of course, defeat the purpose of any benefits derived from VBC if a patient was simply discharged, only to not have their health care needs addressed. Quality of care must be protected. VBC accounts for this by comparing the average length of stay against peer hospitals in similar healthcare environments.
Length of stay is usually not compiled into one large metric to determine the total length of stay for every disease a hospital treats. Instead, it is typically measured against a disease’s total length of stay. This ensures that hospitals that take on more medically complex cases are not penalized for their efforts.
Factors Affecting Length of Stay in Hospital
As noted above, a singular focus on how to reduce the average length of stay in hospitals does not ultimately control costs, as many other factors can impact the length of stay. For example, a focus on only reducing hospital length of stay may result in hospitals seeking to deal exclusively with patients who would have a shorter length of stay. Focusing only on reduced length of stay in hospital is an inadequate health care measure.
Instead, many VBC-based formulas don’t just focus on the length of stay. They also focus on predicting the length of stay in the hospital and then incentivizing hospitals to achieve necessary reductions. They do this by calculating the average length of stay for a particular condition. From there, payments are made based on how a hospital performs at making these discharges.
As you can imagine, managing this type of payment system requires intensive data. Payers need access to data to make accurate payments. Access to this data allows payers to determine how a hospital is performing across a variety of important metrics, including discharge by disease.
Hospitals also need access to this data to monitor patients and make the best care decisions for their patients. With the proper EHR, hospitals can also integrate an EHR with a Clinical Decision Support System—like EvidenceCare—ensuring clinicians are given the best possible information around length of stay.
Hospitals that engage in more frequent discharges can increase bed turnover and better manage capacity. This impacts margins for hospitals and the number of patients they can serve.
The benefits of reducing the length of stay in hospitals are incentivized via a financial formula. In this formula, hospitals are paid more for discharging patients quicker. Doing so typically means better healthcare results. It also reduces the chances of a patient acquiring a hospital-based infection.
A key component of sticking to any VBC-based formula—and improving patient care—must be using the right technology. At EvidenceCare, we offer an array of EHR-integrated CDS software that can assist your hospital in improving outcomes and reducing costs while also enabling you to implement a value-based care model. Our software, CareGauge, specifically helps reduce unwarranted variation and length of stay to promote value-based care best practices.
Want more information? Contact us today to schedule a demo.